When I was a kid one of my neighbors got a hamster. The little critter was super cute and funny and we spent hours playing with him. One morning the hamster was dead., he had been eating and had been very active so the death was unexpected. My neighbors parents being careful took the hamster to a vet and the vet sent a sample to be tested for rabies and to everyone’s surprise, the test came back positive! Needles to say, everybody was upset and worried.
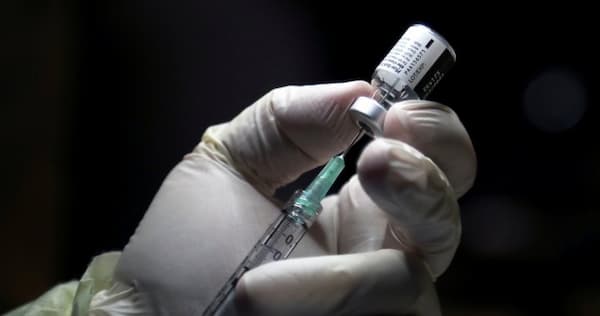
As soon as we had the lab results back my mom took me to the hospital where they started me on the rabies prophylaxis which included a series of injections directly in the abdomen and through the belly button. I don’t remember how many shots I got but it seemed like a thousand of them.
We later learned that the vet had sent a nerve from a leg instead of a sample from the brain which made the test inconclusive. At that same time, my neighbor’s sister confessed that she had dropped the hamster the night before they found that he had died.
Although the whole thing was a pretty negative experience it served to raise awareness about pet vaccination, which was not a huge priority at the time.
In the 2000s Mexico started yearly free rabies vaccination campaigns and in September 2019 Mexico became the first country to be validated by the World Health Organisation for eliminating rabies in humans that has been transmitted by dogs.
When I was in high school a friend invited me to participate in the Rotary’s PolioPlus program. At the time I had not volunteered much without my family or my scout group but it sounded like fun so I signed up.
The aim was for government agencies and NGOs to vaccinate as many children in a single day with the help of more than 300,000 volunteers a dunting but super cool feat if accomplished.
To prepare for the day I reread my school science book that talked about vaccines and whatever was available in our library at home.
We got basic training about setting up the vaccination stations, queues and since the vaccine was the oral polio vaccine (OPV), which was a live, weakened (attenuated) virus given as drops in the mouth, we also got training on what to do in the case of a child spitting out or vomiting after being given the vaccine.
I was really eager to participate but unfortunately the big day was on a Sunday and at that time I was doing my military service, which was pretty much just basic military drills and community service like painting walls or cleaning streets, so I ran the risk of missing all the action. Fortunately my CO was very understanding and he let me go early so I can participate in the big event.
When I arrived everything was set up so I helped to organize the people, give out information and help in whatever else I could. Although it was a long and hectic day all in all was a very positive experience and I am proud of the tiny part I played to help eradicate the horrific scourge of Polio from Mexico.
Volunteering for such a gigantic and important effort was a great and humbling experienced that helped awaken my desire to lend my hand whenever I could to help make the world better for myself and for others.
I have also been lucky to participate in cat and dog rabies immunization campaigns which are super important, specially in locations where pets can be in contact with wildlife.
In Quintana Roo there’s an ongoing rabies immunization campaign and even then there was a human fatality due to rabies in Cancun
PolioPlus program was a Rotary's initiative in polio vaccinations which began in 1985 with the goal of immunizing every child in the world. Mexico was a key part of this effort, and in the late 1980s, Rotary supported National Immunization Days where a campaign was launched to vaccinate 13 million children.
Rotary's involvement in polio immunization began in the Philippines in 1979, which then expanded to Latin America and Mexico in the early 1980’s. The PolioPlus program which officially launched in 1985 had a fundraising goal of $120 million to eradicate polio and By 1987, they had exceeded this, raising $240 million.
Mexico was one of the first countries to have a major immunization day under the PolioPlus program, with 13 million children vaccinated. Local Rotarians helped manage logistics, recruit and train volunteers, and raise funds for materials needed for the immunization days, such as ice boxes and leaflets.
The eradication of Polio in Mexico, culminating in the certification of the Region of the Americas as polio-free in 1994 has had a profoundly positive and transformative impact on the Mexican population, encompassing public health, individual well-being, and the national health system with many positive impacts.
Protection of Children from Paralysis and Death
Zero New Cases of Wild Polio:
Since the last reported case in 1990, generations of Mexican children have been protected from the risk of contracting wild poliovirus, a highly contagious disease that causes irreversible paralysis in approximately 1 in 200 infections.
Prevented Disability and Mortality:
The elimination of the disease means that thousands of children are saved annually from permanent physical disability, which often affects the legs, as was the case of a close relative and a schoolmate of mine, and can necessitate lifelong use of wheelchairs or other assistive devices. It also prevented deaths caused by respiratory failure from paralyzed breathing muscles.
Reduced Healthcare Costs:
The elimination of polio has led to significant long-term economic savings for the country. These savings come from:
- Avoiding the lifelong costs of medical care, rehabilitation, and assistive technology (like iron lungs or braces) for new paralytic cases.
- Freeing up specialized hospital beds and medical personnel who would otherwise be dedicated to treating and managing new polio patients.
Increased Productivity:
Children and adults are able to grow up without polio-related disabilities, contributing fully to society, education, and the workforce, thereby boosting national productivity.
Elimination of Fear:
The eradication removed one of the most terrifying diseases of the 20th century from public life, allowing parents and communities to raise children without the constant fear of sudden, permanent paralysis.
The polio eradication campaign served as a powerful catalyst for improving the overall public health infrastructure in Mexico:
Enhanced Immunization Programs:
The mass vaccination campaigns National Immunization Days and the establishment of a robust national cold chain system to deliver the polio vaccine laid the groundwork for the successful delivery of other childhood vaccines. This strengthened the Expanded Programme on Immunization or EPI, leading to better control or elimination of other vaccine-preventable diseases like measles and rubella.
Improved Disease Surveillance:
The required surveillance system for Polio, which monitored every case of Acute Flaccid Paralysis (AFP, established a highly effective reporting and response network. This infrastructure continues to be used today for tracking and controlling other emerging or re-emerging infectious diseases.
Model for Global Health Efforts:
Mexico's success, particularly its ability to achieve high coverage in remote areas with the help of volunteers, became a model and a source of expertise for other countries embarking on large-scale disease eradication initiatives globally.
In essence, the eradication of polio delivered a lasting legacy of healthier children, a more resilient health system, and tangible economic benefits that continue to accrue decades later.
If you were paying attention in primary school you may remember that the practice of vaccination traces its roots back to the late 18th century, with earlier practices of inoculation having existed for centuries. In 1796 the English physician Edward Jenner developed the world's first successful vaccine against smallpox. Jenner took material from a cowpox sore and used it to inoculate a young boy, who then became immune to smallpox. He called his method "vaccination," taking the name from vacca, the Latin word for cow. This discovery laid the foundation for modern immunology and disease prevention and fundamentally change the fate of humanity.
To date, Smallpox is the only human infectious disease has been completely eradicated globally by vaccination efforts
The World Health Organization (WHO) declared it eradicated in 1980, following a worldwide vaccination campaign.
Polio is on the brink of being eradicated, if idiots decide to stop believing misinformation and vaccinate their kids, with two of the three wild poliovirus types already wiped out. Many other diseases, like measles, mumps, and rubella, have been eliminated in certain regions or countries thanks to vaccines, but they still circulate globally. However, there have been recent outbreaks.
There have been 43 outbreaks reported in 2025, and 87% of confirmed cases (1,401 of 1,618) are outbreak-associated. For comparison, 16 outbreaks were reported during 2024 and 69% of cases (198 of 285) were outbreak-associated (Source CDC).
Herd Immunity, Community Immunity, or Herd Protection
Herd immunity, also known as community immunity or herd protection, is a concept where a population is protected from a contagious disease because a large enough percentage of the individuals are immune.
When enough people are immune, the chain of infection is broken, making it very difficult for the disease to spread to those who are not immune.
Imagine a disease trying to spread through a community.
No Immunity or Open Spread:
If an infected person is surrounded by susceptible people, the disease spreads quickly and widely, like a fire finding dry wood.
Herd Immunity or Protected Community:
If the infected person is surrounded by a high number of immune people, the virus hits "dead ends." It can't jump easily to a susceptible person because the immune individuals act as a protective barrier or shield.
This shield is critical for protecting the most vulnerable members of the community who can't be vaccinated, such as:
- Newborn babies.
- People with weakened immune systems due to medical conditions (like cancer or HIV).
- People with severe allergies to vaccine components.
How Herd Immunity is Achieved
There are two primary ways a population can achieve the level of immunity needed for herd protection:
-
The Safest and Most Effective Way
Vaccines safely teach a person's immune system to recognize and fight a disease-causing germ without having to suffer the illness. When enough people are vaccinated, it starves the germ of new hosts and slows or stops its spread.
This is the preferred public health strategy because it achieves community protection without the widespread sickness, hospitalization, and death that comes with natural infection.
-
Natural Infection (When there is no other choice or people are incurious and uncaring)
Immunity can also be acquired when a person is infected with a disease and recovers. However, achieving herd immunity through natural infection requires a large portion of the population to get sick.
For dangerous diseases, this approach leads to an unacceptable number of severe illnesses and deaths, which is why global health authorities advocate for vaccination.
The Herd Immunity Threshold
The level of immunity needed to protect the community—the Herd Immunity Threshold (HIT) is not the same for every disease. It depends on how contagious the disease is, which is measured by a value called the Basic Reproduction Number (R0) .
| Disease | R0 (Approximate) | Estimated Herd Immunity Threshold |
|---|---|---|
| Measles | 12 - 18 | ∼93% to 95% |
| Polio | 5 - 7 | ∼80% to 85% |
The more contagious a disease, the higher the R0, the higher the percentage of people who must be immune to achieve herd immunity.
The Basic Reproduction Number R0
The basic reproduction number R0, or "R naught," is an epidemiological metric that estimates the average number of new infections generated by one infected person in a population with no prior immunity or interventions.
R0 values are not biological constants; they are estimates that can vary based on the specific strain, location, population density, and study methodology.
Estimated R0 Ranges for Various Diseases
| Disease | Transmission | Estimated $\mathbf{R_0}$ Range |
|---|---|---|
| Measles | Airborne (Aerosol) | 12–18 |
| Chickenpox (Varicella) | Airborne (Aerosol) | 10–12 |
| Mumps | Respiratory droplets | 10–12 |
| Rubella (German Measles) | Respiratory droplets | 6–7 |
| Polio | Fecal–oral route | 5–7 |
| Smallpox | Respiratory droplets | 3.5–6.0 |
| HIV/AIDS | Body fluids (sexual contact, blood) | 2–5 |
| SARS (2003) | Respiratory droplets | 2–4 |
| Common Cold (e.g., Rhinovirus) | Respiratory droplets | 2–3 |
| Ebola (2014 outbreak) | Body fluids | 1.5–2.5 |
| Seasonal Influenza | Respiratory droplets | 1.3–1.4 |
COVID-19 R0 and Variants
The R0 for COVID-19 has varied significantly across its different strains and variants due to increased transmissibility.
| COVID-19 Variant/Strain | Estimated R0 Range |
|---|---|
| Ancestral/Wild-Type (Early Pandemic) | 1.4–6.49 (Mean ≈ 3.28) |
| Delta variant | Mean ≈ 5.08 (Range 3.2–8) |
| Omicron variant | Mean ≈ 9.5 (Range 5.5–24) |
R0 vs. Re Effective Reproduction Number
It's important to distinguish R0 from Re Rt, the effective reproduction number
- R0 is a theoretical measure of a disease's maximum potential for spread before control measures, vaccination, or population immunity.
- Re is the actual number of new infections caused by one existing case at a specific time in a population that is partially immune or under control measures. Public health interventions like masks, social distancing, and vaccines aim to reduce Re to less than 1, which causes the outbreak to decline.
What is mRNA?
Messenger RNA (mRNA) is a single-stranded molecule that plays a central role in gene expression. Its main function is to act as an intermediary messenger, carrying genetic instructions from the DNA in the cell's nucleus to the ribosomes in the cytoplasm, where proteins are made.
Think of it as a chef's recipe:
- DNA is the master cookbook, stored in the nucleus.
- mRNA is a temporary copy of a single recipe (gene) that is carried out to the kitchen (ribosome).
- The ribosome reads the mRNA sequence to assemble the protein (the dish).
The sequence of an mRNA molecule is read in sets of three bases (codons), which each correspond to a specific amino acid, the building blocks of a protein.
Main Landmarks in mRNA Development
The development of mRNA technology, culminating in its use for therapeutics and vaccines, spans over 60 years of fundamental and applied science.
| Year | Landmark | Significance |
|---|---|---|
| 1961 | Discovery of mRNA | Independently confirmed by multiple teams, including Sydney Brenner, François Jacob, and Matthew Meselson, demonstrating that an unstable intermediate molecule carries genetic information from DNA to ribosomes. |
| 1984 | In Vitro Transcription | Researchers developed methods for producing large quantities of functional, synthetic mRNA outside of a cell using an enzyme (T7 RNA polymerase). This made laboratory produced mRNA feasible. |
| 1990 | First In Vivo Protein Expression | Scientists demonstrated that injecting synthetic mRNA directly into the muscle of mice resulted in the mice's cells producing the corresponding protein. This proved the concept for mRNA therapeutics. |
| 2005 | Nucleoside Modification Breakthrough | Katalin Karikó and Drew Weissman discovered that replacing a common RNA building block called uridine with a modified version (pseudouridine) prevents the mRNA from triggering an inflammatory response and significantly increases protein production. This was a critical step in making mRNA safe and effective for therapeutic use. |
| 2012 | Lipid Nanoparticle Optimization | Advances in nanotechnology led to the development of highly effective Lipid Nanoparticles. These fatty bubbles protect the fragile mRNA from degradation and are essential for efficiently delivering it into human cells. |
| 2018-2019 | Advanced Clinical Trials | mRNA vaccines for infectious diseases (like rabies and influenza) began to show promising results in early-stage human clinical trials, validating the LNP/modified-mRNA approach. |
| 2020 | First Approved mRNA Vaccines | The COVID-19 pandemic accelerated development, leading to the emergency authorization and subsequent full approval of the Pfizer/BioNTech and Moderna mRNA vaccines. This was the first time mRNA technology was brought to market, marking a historical validation of the decades of research. |
Risks and Side Effects of COVID-19 Vaccines
The known risks and side effects of the COVID-19 vaccines generally fall into two categories: common, mild side effects and rare, serious adverse events.
Health authorities worldwide, including the CDC and WHO, emphasize that serious side effects are extremely rare and that the known and potential benefits of vaccination for preventing severe illness, hospitalization, and death from COVID-19 significantly outweigh the known and potential risks.
Common, Non-Serious Side Effects
These are signs that your body is building protection and typically last only 1–3 days They are more common after the second dose of the primary series and the booster doses.
| Category | Side Effect |
|---|---|
| Local | Pain, redness, and swelling on injection site |
| Systemic (General Body) | Fatigue, headache, muscle aches, chills, fever, and joint pain. |
| Other | Nausea, vomiting, and swollen lymph nodes (often in the armpit on the same side as the injection). |
Rare, Serious Adverse Events
These are monitored closely by health agencies and occur at very low rates, typically a few cases per million doses administered.
Associated with mRNA Vaccines like Pfizer-BioNTech and Moderna
The primary serious risk associated with the mRNA vaccines is a form of heart inflammation:
Myocarditis or inflammation of the heart muscle and Pericarditis or inflammation of the lining outside the heart.
Risk Profile: These conditions are rare but occur most frequently in adolescent and young adult males (typically ages 12–39), usually within a week after receiving the second dose of the primary series.
Outcome: Most patients who develop this condition after vaccination experience mild illness and recover quickly, often with rest and simple treatments.
Context: The risk of developing myocarditis and pericarditis is substantially higher after getting infected with the COVID-19 virus itself than it is after getting the vaccine.
Anaphylaxis or Severe Allergic Reaction is an extremely rare, immediate reaction to a vaccine ingredient and not to the mRNA itself. Vaccination sites are prepared to treat anaphylaxis immediately.
Associated with Viral Vector Vaccines like Johnson & Johnson/Janssen and AstraZeneca
The primary serious risks associated with the viral vector vaccines are also extremely rare:
- Thrombosis with Thrombocytopenia Syndrome is rare and potentially life-threatening syndrome that involves blood clots combined with low platelet counts (thrombocytopenia).
This has been linked primarily to the Janssen and AstraZeneca vaccines and is more common in younger women.
Due to this risk, the use of these vaccines has been limited or halted in some regions, with health agencies generally favoring mRNA vaccines.
- Guillain-Barré Syndrome is a very rare neurological disorder in which the body's immune system damages nerve cells, causing muscle weakness and sometimes paralysis. A small increased risk has been observed after the Janssen vaccine.
Summary of Risk vs. Benefit
The consensus among major global health bodies is that the benefits of COVID-19 vaccination far outweigh the risks. While the vaccines have rare, associated side effects, the risk of serious complications, long-term health issues, hospitalization, and death is much higher if you become infected with COVID-19 compared to receiving the vaccine.
Ethical Responsibility, Social Contract and Reciprocity
The responsibility of people who benefit from participating in society regarding vaccines is rooted in the ethical concept of the social contract and the duty of reciprocity and beneficence.
In a functioning society, individuals receive numerous benefits such as public safety, infrastructure, education, and public health systems that they can't personally create or sustain alone. This creates a moral responsibility, often framed as a social contract.
The choice to get vaccinated is viewed as a prosocial act and a fair share contribution to the collective benefit of public health, which all members of society rely on. Individuals who benefit from a high vaccination rate or herd immunity have a corresponding duty to help maintain that protection.
Vaccination is a key way to uphold the ethical principle of not causing harm by reducing the risk of transmitting infectious diseases to others. This duty outweighs individual autonomy when an individual's action or inaction poses a significant threat to community health.
Protection of the Vulnerable
The primary ethical duty of vaccination is to protect vulnerable people who cannot be vaccinated or whose immune systems are compromised. These groups cannot cultivate individual immunity and rely almost entirely on the community's high vaccination coverage for their safety.
This includes infants and young children not yet eligible for a vaccine. Individuals with medical contraindications like severe allergies to a vaccine component. People who are immunocompromised including organ transplant recipients and cancer patients for whom the vaccine may be less effective.
Balancing Autonomy and Public Good
While the principle of bodily autonomy is highly valued, public health ethics often prioritizes the greater good of the community. In the context of contagious diseases, the ethical consensus is that individual freedom ends where it significantly and demonstrably poses a risk of harm to the community, therefore, for people who are medically eligible, their responsibility is to get vaccinated to protect both themselves and the community. Base their decisions on scientific evidence and reliable public health guidance, rather than misinformation, to fulfill their obligation to social welfare.
The Politicization of Public Health and Anti Vaccine Movements
The politicization of public health has profoundly impacted anti vaccine movements, transforming vaccine hesitancy from a niche concern into a major issue often aligning with political identity and polarization.
Key Effects of Politicization
The primary link between politics and anti-vaccine sentiment is a divergence in attitudes based on political ideology and party affiliation . Prior to the COVID-19 pandemic, vaccine attitudes were largely apolitical. Since then, especially in countries like the United States, a significant partisan divide has emerged. Those identifying with conservative or right-wing ideologies generally exhibit greater vaccine skepticism, lower trust in public health institutions, and higher rates of vaccine hesitancy compared to those identifying as liberal or Democrat. Negative attitudes initially focused on the COVID-19 vaccine have spilled over to other, well established, and unrelated vaccines, such as those for influenza, measles, mumps, and rubella. This suggests the resistance is now often rooted in political identity rather than specific safety concerns about a single vaccine . Anti vaccine sentiment often aligns with anti establishment and "personal liberty" values, where government mandates are viewed as an infringement on individual freedom. Political rhetoric emphasizing these themes can amplify distrust in institutions like the CDC and major pharmaceutical companies . Political polarization is reinforced by differential media consumption. People with conservative leanings are more likely to consume news sources that promote mistrust, misinformation, or conspiracy theories about vaccines, which increases their hesitancy .
Impact on Public Trust and Policy
The politicization of vaccines has critical consequences for public health:
Political rhetoric that questions the motives, data, and decisions of public health officials and scientists directly erodes public trust in these institutions, making it difficult to achieve consensus on public health policies . Political polarization can undermine the effectiveness of public health regulations, making compliance lower in regions where the public views the government's stance as ideologically opposed to their own . Studies have shown a correlation between higher political opposition to vaccines and lower vaccination rates, which can, in turn, lead to higher rates of infection and death in those areas during infectious disease outbreaks .
The politicization essentially recasts a medical decision as a political statement and part of a person's identity, driving anti vaccine movements to greater prominence and greater impact on collective health.
The contemporary anti vaccine movement is a clear example of irresponsible science denialism, sharing a fundamental characteristic with fringe beliefs like Flat Earth theory. Both movements prioritize personal ideology, distrust of authority and experts, and selective misinformation over overwhelming scientific consensus. To reject vaccines, which are a foundational public health triumph based on rigorous immunology and epidemiological data, is to engage in a denial of established, life saving knowledge. Such arrogance and irresponsibility threatens not only individual health but also collective wellbeing by endangering herd immunity and potentially causing the resurgence of preventable diseases. Ultimately, the anti vaccine stance is a form of willful ignorance that dangerously disregards the scientific method and public safety for the sake of political or personal contrarianism.